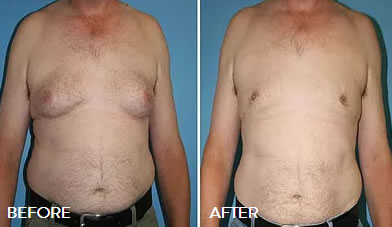
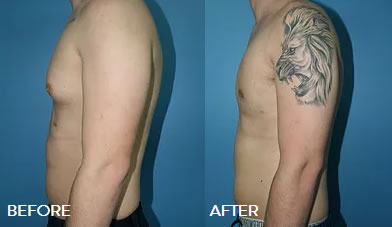
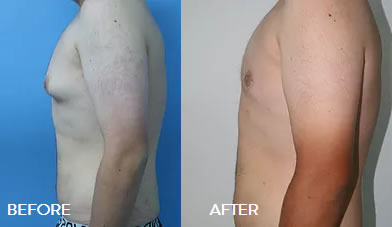
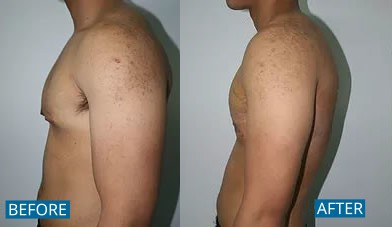
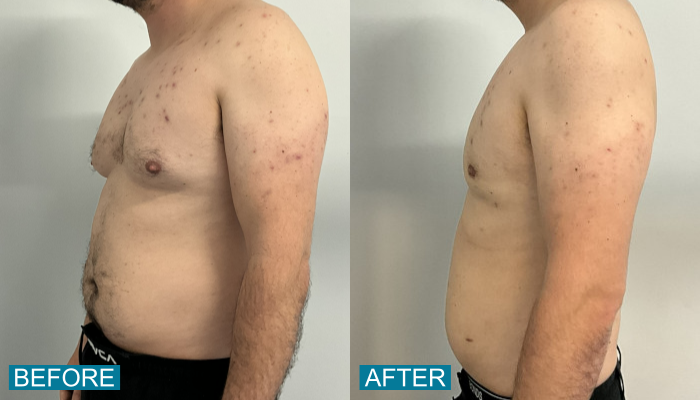
Breast reduction is not a subject that is often associated with men, however, excess breast tissue or fat in one or both breasts affects an estimated 40 to 60 percent of men.
While certain drugs and medical conditions can contribute to breast overdevelopment, most cases do not have a known cause.
If you are considering surgery for gynecomastia, our Frequently Asked Questions below will help you to understand the procedure.
Frequently Asked Questions
Male breast reduction surgery can be performed on men of any age who are in good physical and emotional health. The best candidates for this surgery have firm skin with sufficient elasticity to adapt to the body’s improved contours.
The initial consultation with your surgeon will require your complete medical history, so you will want to be prepared to provide the necessary information. Your surgeon will examine your breasts and discuss lifestyle issues which may be causing your condition. You must be completely open and honest with your surgeon. Dr McHugh will assess your physical and emotional health, discuss your aesthetic goals, and address any questions or concerns you may have.
This consultation is also the time to ask all of your questions about the treatment and costs. If you have health insurance, treatment of Gynecomastia may be covered.
Issues you should be prepared to discuss during consultation with Dr. McHugh include:
– Your specific aesthetic goals
– Medical conditions, both past and present
– Current medications, including nutritional supplements and herbal remedies
– Past surgeries
As with all cosmetic surgery, results will be rewarding if expectations are realistic. Like any surgery, there are some risks that Dr McHugh will discuss with you.
Our clinic is conveniently located in Penrith. Simply contact us at our clinic on 02 4721 8838 to schedule an appointment.
Treatment for gynecomastia is dependent on the type of gynecomastia. Dr McHugh will help you choose the technique best suited for you based on your presentation.
PSEUDOGYNECOMASTIA
Liposuction or liposculpture of the pseudogynecomastia is used to remove the fatty tissue by suction using a negative pressure source (pump or syringe). Usually performed with tumescent method to decrease bleeding.
GYNECOMASTIA
Excision of the male breast tissue. This real gynecomastia tissue cannot be suctioned and has to be removed by surgical excision – male breast reduction. Usually performed through the lower part of the aerola (between the pigmented part and the skin). When done properly, this usually leaves inconspicuous scars (athletes and body builders cannot afford prominent scars).
COMBINED PSEUDOGYNECOMASTIA AND GYNECOMASTIA
The treatment of choice is a combination of surgical excision and liposuction for men (for better breast contour).
SEVERE GYNECOMASTIA
For ease of understanding, we will compare the male breast size to the female breast size (A, B, C, D, DD, etc.) and as such, there are a few modalities of treatment available:
– Periaureolar (incision around the nipple aureola complex) male breast reduction: this procedure is meant for mild to moderate reductions. This can be compared to size A and B in women
– Classical breast reduction with superior or inferior flaps: this is for larger breasts (C, D) and leaves an inverted xTx incision and periaurieolar incision. It is used very rarely
– Vertical incision breast reduction that results in a vertical subareolar scar (not horizontal scar) in large breasts: this is a new alternative
Though thousands of men undergo gynecomastia correction each year and experience no major complications, the procedure does carry some degree of risk.
It is important that you be well informed of these risks when considering surgery. The discussion of potential risks and complications is one of the most important aspects of patient consultation. During your consultation, Dr McHugh will discuss these potential complications with you, listen to your safety questions, and offer recommendations on how to minimise your risk.
Certain specific risks of male breast reduction surgery:
– When male breast reduction is performed by an experienced cosmetic surgeon, complications are infrequent.
– Scarring can be minimised when the incision is done correctly and in the proper location. Generally, noticeable scarring is minimal. Should adjustment be necessary, this can be done using several treatment modalities at a later date.
– Hypoesthesia (reduced areola sensation). This condition usually improves within six months post-surgery.
– Areola or breast depression:
– Static – Can be seen when the pectoral muscle is relaxed. This is the most severe form and sometimes requires correction
– Dynamic – Can be seen only when the patient lifts his arm or flexes the pectoral muscle. This is usually less bothersome to the patient
– Correction for these conditions:
– Fat transfer
– Fat and dermis transfer
– Injection of Radiance, etc
– Recurrence of the breast tissue occurs, according to recent literature on the subject, 10% after excision and 35% after male liposuction only.
– Patients who have large areolas prior to surgery: This can be addressed during surgery in several ways:
– Adequate thinning of the areola. In many cases this is enough to reduce the size
– Purse string sutures of the areola and nipple complex
– Surgical excision of the areola, which is rarely performed
– Hematoma and Seroma: this accumulation of blood and blood products may cause excessive swelling of the breast after the Gynecomastia treatment surgery which sometimes requires intervention. This occurs more often in patients who:
– Suffer from high blood pressure
– Take aspirin or blood thinners prior to surgery
– Take certain food supplements
– Take anabolic steroids prior to surgery
– Do not follow postoperative instructions
It is important to follow Dr McHugh’s instructions when preparing for surgery to ensure the best possible results. Those instructions may include:
– Refraining from smoking for several weeks before and after surgery
– Avoiding certain medications
– Arranging for help following surgery, such as a ride home and in-home care for the first 24 hours after you leave the hospital
For your comfort and convenience, Dr McHugh operates either in his clinic under local anaesthetic with intravenous sedation or under general anaesthetic at various private hospitals.
He will carefully monitor your physical status throughout the operation and during your recovery.
It is normal to feel some discomfort for a few days after your procedure. This can be controlled with medication prescribed by your surgeon.
You should arrange to be driven home after your surgery and have someone to help you manage for a day or two if necessary.
Bruising and swelling may make it appear that there’s been no improvement in your condition initially. You will most likely be told to wear an elastic pressure garment around the clock for a week or two, and for several weeks longer at night. The extreme swelling will resolve in the first few weeks but it may be three months or longer before your true result is visible.
While you are waiting for this, it is important to begin to resume normal activity. You should walk around on the day of surgery, and return to work within a day or two, as soon as you feel well enough. If you have stitches, they will be removed one to two weeks after the surgery.
You should avoid sexual activity for a week or two, and heavy exercise for about three weeks. You must avoid any activity or job that risks a blow to the chest area for at least a month. Avoid exposing scars to the sun for at least six months. Sunlight can cause the scar to darken permanently. If sun exposure is unavoidable, use a strong sunblock.
If you went into gynecomastia correction with realistic expectations, you’ll most likely be very pleased with your results.
Though gynecomastia correction provides long-lasting enhancement, it is important to remember that issues such as age, genetics and weight fluctuation can change the size, shape and position of even enhanced breasts over time.
Follow-up visits are important to answer any questions you may have and monitor your healing process. Your first post-operative visit will be scheduled after the initial healing period, during the first few days after surgery.
In the following months, Dr McHugh may ask you to return for periodic checkups. Keeping these appointments is important to assess your long-term results and address any questions or concerns you may have.
Gynecomastia Gallery

His dual specialisations enable him to deliver excellence in surgical results, with an eye for aesthetic beauty.
With over 20 years of experience as a surgeon in the private sector and performing international aid work as a Surgeon Commander with the Royal Australian Navy, you can have confidence that Dr McHugh is uniquely qualified and trusted to deliver the results you seek.